Urticaria, also known as hives or welts, are itchy, raised, 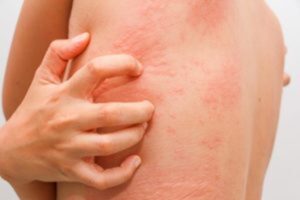 red or skin-colored bumps that appear on the surface of the skin. Hives typically blanch (turn white) when pressure is applied and can vary in size and shape.
red or skin-colored bumps that appear on the surface of the skin. Hives typically blanch (turn white) when pressure is applied and can vary in size and shape.
When swelling occurs in the deeper layers of the skin, it is called angioedema. Angioedema typically affects the face (eyelid, lips, and tongue), hands, or feet, and can occur with or without hives.
What causes hives?
The underlying mechanism for hives lies with a specialized cell called the Mast Cell. Mast cells are found throughout the body, including the surface of our skin. When these mast cells are stimulated, they release histamine and other allergic mediators that cause hives and swelling.
Triggers for mast cell activation can include:
- Allergic reactions (food, medications, insect stings)
- Viral or other infections
- Physical factors (heat, cold, pressure, exercise)
- Autoimmune processes
- Unknown triggers
Urticaria can be broadly classified as either acute or chronic.
Acute hives
Acute hives are relatively common and affect up to 25% of people at some point in their life. Acute hives are self-limited, typically resolving within a few hours to a few weeks. This category of hives resolves within less than 6 weeks and can occur in any age group. Acute hives are often one-time or situational in occurrence.
Common causes:
- Viral infections (most common cause, especially in children)
- Foods
- Medications
- Insect stings
- Physical triggers (rapid changes in temperature, heat/cold)
Diagnosis involves a thorough history, physical exam, and testing to help identify the cause of the hives. Treatment may include non-sedating oral antihistamines to control itching and avoidance of known triggers, if identified.
Chronic hives (Chronic Spontaneous Urticaria)
Chronic hives are less common and affect less than 5% of people at some point in their life. Chronic hives are defined as hives that occur on most days of the week and persist for more than 6 weeks. They are more common in adults, especially women, but can occur in children as well. Chronic hives tend to reoccur.
Key Facts:
- About 40% of people with chronic hives will also experience angioedema
- In 80-90% of cases, no clear, specific cause can be identified
- Most cases are not caused by a dangerous underlying disease, though a specific trigger often cannot be identified
- The most common identifiable cause is due to an autoimmune mechanism
- It’s common, not alarming. About 1 in 5 patients with chronic hives has autoimmune thyroid disease (most often Hashimoto thyroiditis), and 10–28% have at least one autoimmune condition overall. This is a well-recognized association, not a sign that something is going seriously wrong.
In autoimmune forms, the body may produce autoantibodies that target the thyroid gland, the IgE (the allergy antibody), or the high-affinity IgE receptor on mast cells. Based on the clinical presentation, diagnostic testing may be necessary to help identify and/or rule-out any underlying disease process that could be associated with the hives.
What chronic hives are usually NOT caused by
Unlike acute allergic reactions, chronic hives are usually not caused by:
- seasonal allergies
- pet allergies
- foods
- detergents or soaps
This is one of the biggest misconceptions patients have about chronic urticaria.
Common Triggers for Both Acute and Chronic Hives
- Stress: Emotional or physical stress can induce histamine release.
- Skin Irritation: Tight clothing, friction, or scratching (dermographism).
- Physical Stimuli (heat, cold, pressure)
- Heat/sweating (hot showers/baths)
- Exercise
- Alcohol
- Infections
- Medications (NSAIDs, antibiotics, opioids, contrast dyes)
- Sleep deprivation/fatigue
When are hives an emergency?
Seek immediate medical attention if hives occur with:
- trouble breathing
- throat tightness
- tongue swelling
- dizziness or fainting
- vomiting after allergen exposure
These symptoms may indicate Anaphylaxis.
Treatment of Chronic Hives
Treatment for chronic hives is typically stepwise and starts with daily antihistamines. Dosing may be increased under medical guidance if symptoms persist. There are also a few other medications which may be added for improved response.
First-line treatments:
- Daily second-generation (non-sedating) antihistamines, such as:
- Xyzal (levocetirizine)
- Zyrtec (cetirizine)
- Allegra (fexofenadine)
- Claritin (loratadine)
- Adjunct therapy options:
- Pepcid (famotidine) is a histamine H2 blocker and common acid suppressor, which may be added in some cases, though their benefit is variable
- Singulair (montelukast), which is a leukotriene modifier that has anti-inflammatory properties that may help with hives in some cases
Often, these first line medications control chronic hives. If there is inadequate response and breakthrough symptoms are occurring, additional treatment options are available.
Short-term treatments
- Sedating antihistamines such as Benadryl (diphenhydramine) and Atarax (hydroxyzine). Some patients, however, do not respond to these medications and long-term use should be avoided due to side effects
- Oral corticosteroids, such as prednisone, may be used for a short course in severe flares, but have numerous undesirable side effects and are not recommended for routine or long-term management of hives
Second-line treatments:
- Biologics such as Xolair (omalizumab), Dupixent (dupilumab), and Rhapsido (remibrutinib). Biologics are safe, long-term medications that are effective for chronic hives.
Third-line treatments:
- Immunosuppressant medications, such as cyclosporine, are effective, however they have undesirable side effects and are therefore reserved for severe, treatment-resistant cases.
If high-dose antihistamines are ineffective for sufficient relief, or if frequent oral steroids are needed, biologics can be a treatment option.
Xolair (omalizumab)
Xolair is an injectable biologic medication originally approved by the FDA for asthma in 2003 and later approved in 2014 for chronic hives. Xolair is also approved for the treatment of chronic rhinosinusitis with nasal polyps (CRSwNP) and for reducing allergic reactions to IgE-mediated food allergies.
Like many other biologic medications, Xolair is a monoclonal antibody that works as an “IgE blocker” – it binds to the allergy antibody IgE and forms a complex which is then eliminated from the body. Xolair binds to IgE before IgE attaches to the mast cell. It also reduces the IgE receptors on the surface of mast cells. The result – less stimulation of mast cells and less release of chemicals that cause hives, itching, and swelling. Therefore, the symptoms and frequency of chronic hives are decreased.
Key Points:
- Approved for patients 12 and older with chronic hives
- Given as a subcutaneous injection every 4 weeks at home or in office
- Approximately 70-75% of patients have symptom improvement, many significantly
- Many patients achieve complete symptom resolution
- Overall safety profile has been favorable in clinical trials
Safety:
- The most common side effect is injection site reactions
- Other side effects reported include upper respiratory symptoms like congestion, runny nose, headaches, and sore throat
- Serious adverse reactions occurred in less than 1% of patients
- Rare risk of anaphylaxis (~0.1%), so initial doses are monitored in office
- Pregnancy registry data is reassuring, but use should be individualized
Dupixent (dupilumab)
Dupixent is another injectable biologic medication, originally approved by the FDA in 2017 for atopic dermatitis (eczema). It then got approved for chronic hives in 2025. In addition to these indications, this medication is also approved for asthma, eosinophilic esophagitis (EoE), prurigo nudularis, bullous pemphigoid, allergic fungal rhinosinusitis, chronic rhinosinusitis with nasal polyps (CRSwNP), and chronic obstructive pulmonary disease (COPD)
Dupixent binds to the interleukin 4 (IL-4) receptor alpha subunit, which stops the inflammatory signals from the proteins: IL-4 and IL-13. These proteins stimulate inflammation. Inhibiting these proteins leads to a reduction in the overactive immune response (mast cell activation), which leads to less itching, redness, and hives.
Key Points:
- Approved for patients 12 years and older with chronic hives
- Given as a subcutaneous injection every 2 weeks at home
- Approximately 40-50% of patients have well controlled symptoms
- 30% of patients achieve complete symptom resolution
- Generally well tolerated and based on clinical studies, very safe
Safety:
- The most common side effect is injection site reactions
- Other side effects reported include conjunctivitis, and joint pain
- Rare risk of anaphylaxis (~0.1%), so initial doses are monitored in office
Rhapsido (remibrutinib)
Rhapsido is an oral biologic medication approved for chronic hives by the FDA in September 2025. It works by blocking the Bruton’s tyrosine kinase (BTK) protein. This protein is found within mast cells and basophils. Blocking this protein prevents the release of histamine and other inflammatory mediators. The result – less hives, itching, and swelling.
Key Points:
- Approved for patients 18 and older with chronic hives
- Is an oral tablet that is taken twice daily, with or without food
- Improvement may be noted as early as 2 weeks
- Approximately 50% of patients achieve well-controlled symptoms after 12 weeks
- 30% of patients achieve complete symptom resolution after 12 weeks
- Generally well tolerated and based on clinical trials, safe
Safety:
- The most common side effects include nasal congestion, sore throat, runny nose, and headaches.
- Lesser common side effects included nausea and abdominal pain
- In clinical trials, 9% of patients experienced bleeding. The most common types of bleeding were petechiae (pinpoint red or purple dots in the skin) and bruising. These were both mild and temporary. There were no reports of severe bleeding within the 24-week trial.
- If you plan to have surgery, your health care provider may tell you to stop taking Rhapsido for 3 to 7 days before and after any procedures
FAQ
Can stress cause hives?
Yes. Emotional stress can worsen mast cell activation and trigger or worsen hives in some patients.
Are chronic hives dangerous?
Most chronic hives are not dangerous, though swelling or severe symptoms should still be evaluated.
Can hives be autoimmune?
Yes. Chronic hives can be associated with autoimmune activation.
How long do chronic hives last?
Some cases resolve within months, while others can persist for years.
What’s the next step?
If you or someone you know has experienced hives, the first step would be a thorough history and physical examination. Allergy testing may be done to rule out allergic causes of the hives. Blood work may be obtained to help identify and rule out causes for chronic hives. If oral medications are not controlling the hives, Xolair, Dupixent or Rhapsido may be a safe long-term option for you to help reduce the frequency and severity of symptoms of chronic hives.
We’re here to help
Our physicians at North Texas Allergy & Asthma Center are board-certified allergists with extensive experience in both pediatric and adult patients with urticaria. We offer comprehensive evaluation and advanced treatment options, including biologic therapies, to help you find relief and improve your quality of life.
Call our office at 940-382-4142 to schedule an appointment – we’re here to help make you feel better!
SHIKHA MANE, MD
Board Certified Allergist







